Pulmonary Disorder Treatment Northern Virginia
What is a Pulmonologist?
A pulmonologist is a specialist in the field of medicine that focuses on diagnosing and treating lung and breathing disorders. Many times lung disorders and sleeping disorders go hand-in-hand.
There is specialized training from medical school to fellowship that is completed in pulmonology and there are board certification exams to complete after fellowship to maintain certification in the specialty.
What Conditions Does a Pulmonologist Treat?
At NOVA Pulmonary Critical Care and Sleep Associates we manage and treat a variety of pulmonary disorders including:
- Pulmonary disorders
- Cough
- Shortness of breath
- Wheezing
- Asthma
- Chronic Obstructive Pulmonary Disease (COPD)
- Emphysema
- Pneumonia
- Bronchitis
- Allergic rhinitis
- Lung Nodules
- Lung cancer
- Sarcoidosis
- Bronchiectasis
- Pleural effusion
- Pulmonary Fibrosis
- Pulmonary Hypertension
- Hypoxia (low oxygen level)
- Pre-operative pulmonary clearance
- Pre-employment pulmonary evaluation
- Occupational Lung Diseases
Asbestosis


The pulmonologist begins the diagnostic process with a general review focusing on family history of diseases affecting the lungs, like cystic fibrosis, or environmental exposures. In addition, other symptoms of disorders may appear in a full-body exam. Often we work with other specialists, like cardiologists, to give a full diagnostic picture of your lung health.
In our office we may take blood tests, spirometry of maximum airflow, Pulmonary Function Tests, Bronchoscopy, Chest X-rays or CT scanning or sleep studies (polysomnography) to determine the ultimate diagnosis.
Patient comfort is of the upmost importance to our practice. We have technologies in our office that allow patients to do at home testing for diagnostic purposes and also are conveniently located next to Stone Spring Hospital for in patient treatment or testing if necessary.
Learn more about Dr. Aditya Dubey, our services, and the treatment of sleep disorders out of his office near Dulles Airport and Stone Springs Hospital in Sterling Virginia.
Questions? Contact NOVA Pulmonary Critical Care and Sleep Associates, LLC
Cough is a widespread symptom resulting from a healthy reflex of the respiratory tract meant to clear the airways. It is sometimes a transient, mild, and self-limited symptom, but depending on its severity and quality, it can be relevant to diagnose significant health problems.
Common causes can be divided into acute cough and chronic cough.
Acute cough is limited to a short period, usually 15 days or less. It may have a sudden or insidious onset, and common causes include infectious and allergic diseases.
- Common cold and other respiratory infections: Most infectious diseases of the respiratory tract feature either dry or productive cough. In the latter, the sputum can be transparent or contain pus and debris (1).
- Croup: It is more common in children, and caused by a viral infection. Patients with croup experience respiratory distress, a hoarse voice, and the onset is often abrupt and tend to worsen at night. The symptoms won’t usually last for more than 2 days, but these patients often need medical attention to recover faster (2).
- Asthma: It is a common respiratory condition that involves allergic reactions and inflammation of the airways. The inflamed airways are narrow, patients display a wheezing sound when breathing in, and the cough reflex becomes activated (3).
- allergies: Seasonal allergies often cause wheezing and cough as predominant symptoms. It can be a consequence of allergic rhinitis, and a transient reflex to prevent aspiration of foreign particles and substances into the respiratory tract (4).
Chronic cough is diagnosed when this symptom is reported for 8 weeks or more. It is usually caused by a complication of another health problem, or as a result of medications for chronic diseases.
- Gastroesophageal reflux disease (GERD): In GERD, acid reflux causes irritation in the esophagus and significant inflammation. Acid reflux may also affect the larynx, causing a hoarse voice and cough (5).
- Chronic obstructive pulmonary disease (COPD) and Asthma: It is a consequence of long-term exposure to irritants of the respiratory tract. The most common cause is cigarette smoking, and patients develop a chronic productive cough that is usually aggravated in the morning (6).
- Upper Airway Cough Syndrome(UACS): Caused by environmental allergens
- Medications for chronic disease: Certain medications for chronic diseases may cause cough as a side effect. The most common is angiotensin-converting enzyme inhibitors (ACE inhibitors). They are drugs used to lower blood pressure in patients with hypertension (8).
Cough is a common complaint, and it is usually diagnosed by considering the characteristics of the symptom, other accompanying signs and symptoms, a complete blood count, and an X-Ray. Viral infections will be treated with support measures to relieve the symptoms, bacterial infections are treated with antibiotics, and allergic conditions can be treated with corticosteroids, nebulization, and inhaled medications.
In some cases, repeated episodes of acute cough and cases of chronic cough should be evaluated by a pulmonologist, a specialist in the lungs, and the respiratory tract. He will be able to assess and follow-up complicated cases, do Pulmonary function test and provide appropriate treatment to control cough and other symptoms associated with the respiratory tract.
Chronic obstructive pulmonary disease or COPD is a lung disease that makes breathing difficult.
It is a long-term disease that often gets worse over time and is characterized by inflammation and severe limitation of airflow in and out of the lungs.
COPD is an umbrella term used to describe a group of breathing conditions, the most common being chronic bronchitis and emphysema. Many people living with COPD may have both emphysema and chronic bronchitis, and a few people have both asthma and COPD.
CAUSATIVE FACTORS:
- Cigarette smoking
- Long-term exposure to secondhand smoke or irritants such as air pollution dust or workplace fumes and biomass exposure such as wood smoke can also contribute to COPD.
- A rare genetic disorder called alpha-1 antitrypsin deficiency is sometimes associated with COPD.
- Respiratory infections such as influenza and pneumonia do not cause COPD, but they worsen the symptoms of COPD.
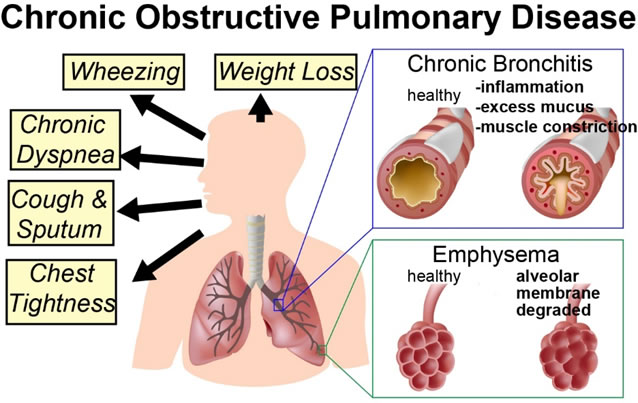
SYMPTOMS:
- Shortness of breath (Dyspnea)
- Wheezing
- Chest tightness especially with exercise
- Persistent cough, often with a lot of mucus.
- With worsening symptoms, simple physical activities become harder and may lead to fatigue weight loss and muscle loss.
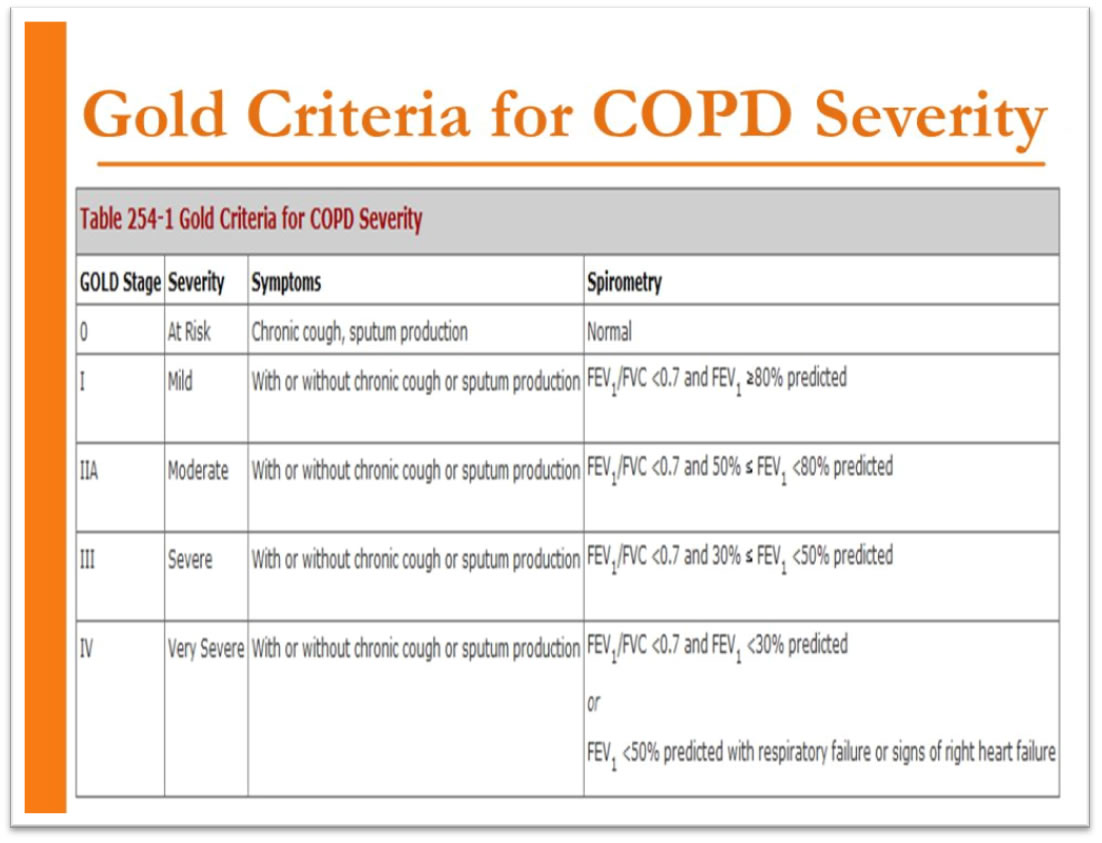
Global Initiative for Obstructive Lung Disease (GOLD) Criteria for COPD assesses various stages of COPD and recommends treatment options accordingly.
The four stages of COPD are:
- Mild: Infrequent cough with mucus, usually un-noticeable symptoms.
- Moderate: Significant shortness of breath.
- Severe: Dyspnea becomes worse, normal exercises become impossible, frequent exacerbation of symptoms.
- Very severe: The quality of life becomes very poor.
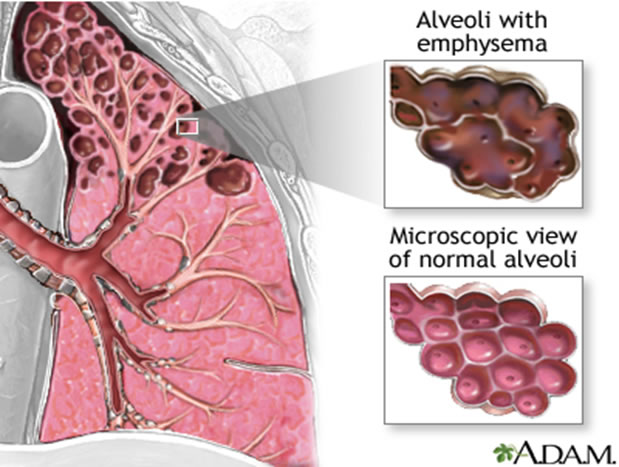
In normal functioning lungs, when air is inhaled, it travels down the windpipe and into the airways or bronchial tubes of the lungs. Inside the lungs, the airways branch out into minute tubes called bronchioles. At the end of these tubes are billions of tiny air sacs called alveoli. The walls of the airways and air sacs are elastic and flexible in nature. Inhalation causes each alveolus to inflate, while exhalation causes each alveolus to deflate. Efficient uptake of air into the lungs supplies oxygen to the blood which is then carried to all parts of the body. In COPD, however, the airways become thick and inflamed and produce more mucus than usual. This mucus can clog the airways, thus making it hard to breathe. In COPD the walls of the air sacs in the lungs are damaged and lose their elastic quality, thus making breathing difficult.
COPD is the third leading cause of death in the USA, affecting approximately thirteen and a half million Americans. The death ratio in women is seen higher than men.
Lifestyle modifications, early consultation, quitting smoking, pulmonary rehabilitation therapy, regular exercise and treatment in consultation with a Pulmonologist can all help in the management of COPD.
(n.d.). Retrieved from https://www.biophysics.org/blog/molecular-mechanisms-of-inflammatory-signaling-in-copd
(n.d.). Retrieved from https://medlineplus.gov/ency/article/000091.htm
(n.d.). Retrieved from https://hirupm.blogspot.com/2019/06/copd-gold-fev1fvc.html
Albert Rizzo, MD, chief of pulmonary and critical care medicine, Christiana Care Health System, Wilmington, DE. . (n.d.).


NOVA Pulmonary – Dulles
24430 Stone Springs Boulevard
Suite 200
Dulles, VA 20166
NOVA Pulmonary – Lansdowne
19415 Deerfield Avenue
Suite 301
Landsdowne, VA 20176
Office Locations
Conveniently located near you in Loudoun and Fairfax VA
NOVA Pulmonary – Dulles
24430 Stone Springs Boulevard
Suite 200
Dulles, VA 20166
NOVA Pulmonary – Lansdowne
19415 Deerfield Avenue
Suite 301
Landsdowne, VA 20176
NOVA Pulmonary – Vienna
124 Park Street SE
Suite 203
Vienna, VA 22180
